At just 25, Jasmine O’Donoghue had life-changing surgery to treat her lymphoedema and now, for the first time in over a decade, she’s doing long bushwalks, travelling overseas comfortably – and she’s even taken up the five-kilometre Park Run challenge.
In November last year, through Macquarie’s ALERT lymphoedema clinic, O'Donoghue underwent surgical liposuction to reduce the persistent swelling in her left leg that had hindered her since she was 12.

Domino effect: Lymphoedema can impact on overall health, says Professor John Boyages.
“On any given week, I will go for walks, jogs, cycle, play tennis, swim and do weights and on weekends I try to explore somewhere new,” she says.
“My left leg used to be 20 per cent larger than the right and by my six-week check-up, it was only 3.6 per cent bigger.”
O'Donoghue’s lymphoedema began with a persistent swelling in her left leg, an outcome of the surgery that removed a malignant melanoma that first appeared as a dark mole on O'Donoghue’s hip when she was just 12.
The cancer had spread to her lymph nodes but after two operations, O’Donoghue was pronounced clear of melanoma.
Lymphoedema, however, is a lifelong progressive condition, often beginning with slight swelling which gradually escalates.
“By today's standards my lymphoedema really wasn't managed very well at all and it took me many years to find the right treatment and eventually the stockings which I'm in now, and by then my left leg was about 20 per cent bigger than my right,” she says.
Professor John Boyages, director of the ALERT lymphoedema program at Macquarie, says the condition is often unrecognised in the general community and there is a lot of uncertainty around treatment.
The early stages of lymphoedema can last for months or years and symptoms may not be obvious. Traditional treatments include exercise, massage, skin care, limb elevation and the continual wearing of expensive compression stockings, which aren’t subsidised by Medicare.
Increased medical and therapist consultations get minimal rebates and soon add up, and patients also have trouble finding clothes or shoes to cater for the swelling, says Boyages.
“It can have a domino effect on the body; people develop arthritis from lifting a heavier limb, they put on weight because they can’t exercise, they end up with frequent hospital visits because of infections, so it affects their overall health, self-esteem, their lifestyle and their finances,” he says.
The chance to be active again
O’Donoghue was an active teenager who had survived cancer and wanted to get on with her life, but her leg continued to swell.
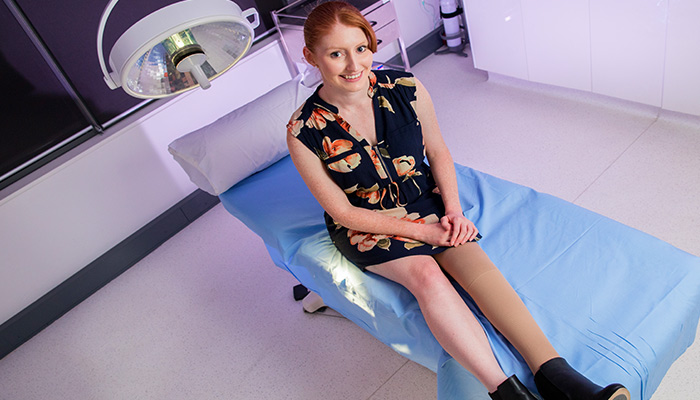
Life-changing: Lympheodema patient Jasmine O'Donoghue at Macquarie's ALERT clinic.
“I avoided sport and eventually cut out any activities which would involve a lot of walking or being on my feet for a long time – including my part-time job,” she recalls.
She avoided wearing shorts or skirts when meeting new people, and shoe shopping often ended in tears because she struggled to find shoes to fit both feet – and the few shoes that fit her were ugly, she says.
Lymphoedema patients often experience infection. The characteristic swelling – which can be in a leg or arm, the neck or even the abdomen – comes from an overflow of the lymph fluid which circulates in the body to remove wastes and bacteria.
“Not long before my HSC I had my first bout of cellulitis,” O’Donoghue recalls. As the condition progressed, infections became more regular. “I adjusted to plan my life and study habits with the knowledge that at any time, I could have to drop everything, go to hospital and then spend a couple of weeks recovering.”
Determined to keep active, O’Donoghue took up swimming and weights, and had decided she would have to "just get on with it", but lymphoedema continued to restrict her.
She was assessed for treatment by the ALERT clinic and joined a health fund, waiting a year for treatment that she could not otherwise afford.
During that waiting time, an infection that began on the first day of a holiday to Queensland in 2017 marked the start of a spate of poor health for O'Donoghue. “I hadn’t done anything particularly risky, it was just a hot day,” she says. “For the next six months I had five infections, some triggered by as little as standing up for a couple of hours.”
O'Donoghue says that treatment at Macquarie’s ALERT clinic has been life changing. She lost four kilograms over the seven months following her surgery. “I've been able to try new hobbies such as bushwalking, jogging and tennis with friends,” she says.
“And then there's the confidence that comes with feeling better about how I look and being able to wear what I want – shiny new heels included!”
ALERT clinic breakthrough treatments
“As a radiation oncologist treating patients with breast cancer, I sometimes cause lymphoedema in the course of treatment, though of course we try to avoid that,” says Boyages.
He heads MQ Health's ALERT program, which combines not-for-profit lymphoedema research and education with a world-class clinical service.
The clinic uses a new technique to work out how much damage there is in lymphatic vessels, by injecting a green dye into the person’s swollen limb and scanning the vessels.
Some patients with early-stage lymphoedema can be helped with lymph node transplants, which surgically transfers lymph nodes from an unaffected area of their own body. The procedure is sometimes done together with surgical breast reconstruction following breast cancer.
Another surgical procedure used to treat early-stage lymphoedema, called Lymphovenous anastomosis (LVA), involves precise micro-surgery to divert a lymph vessel close to the swelling by making several connections joining it to a nearby vein, bypassing the damaged area and allowing lymph fluid to flow back to the venous system.
In patients where lymphoedema has progressed, the ALERT clinic is the first in Australia to use liposuction to remove excess fatty tissue that builds up in the swollen limb. It’s this surgery that gave O'Donoghue a new lease on life.
“We’ve seen lymphoedema that’s been triggered by surgery, industrial and vehicle accidents, pregnancy and it can be genetic,” says Boyages.
“With cancer treatments becoming more effective, we’re now seeing many people who survive cancer, only to be confronted with this lifetime condition.”
Nearly half of the patients treated at ALERT come from outside NSW and overseas, he says.
“We have an international reputation, as the ALERT clinic is one of the few places in the world with this combination of treatments underpinned by research and education. It’s great that we can give people hope.”
